Home » Tips and Tricks » Activities of Daily Living (ADL) » What are the Activities of Daily Living?
Imagine suddenly being unable to bathe yourself, prepare a meal, or manage your medications. For many individuals facing health challenges or aging, losing the ability to perform Activities of Daily Living is like falling down a steep slope – each lost capability represents another step away from independence.
Understanding ADLs isn’t just academic; it’s essential for maintaining dignity and quality of life for vulnerable populations. This guide explains these critical functions and how healthcare professionals assess and support them.
The term “Activities of Daily Living” or ADLs for short is a term used to describe the fundamental skills required to taking care for oneself independently, such as eating, bathing, and mobility. The term “Activities of Daily Living” was first coined by Sidney Katz in 1950.
According to the book “Activities of Daily Living” by Peter F. Edemekong[1], ADLs are essential and routine tasks that most young, healthy individuals can perform without assistance. The inability to accomplish essential activities of daily living may lead to unsafe conditions and poor quality of life.
The healthcare team should be aware of the importance of assessing ADL in patients to help ensure that patients who require assistance are identified. This activity details the activities of daily living and highlights the role of the interprofessional team in assessing ADLs to enhance patient care and management.
The screening of ADLs is performed at two levels, namely Basic ADLs and Instrumental ADLs. The former is commonly referred to as just ADLs.
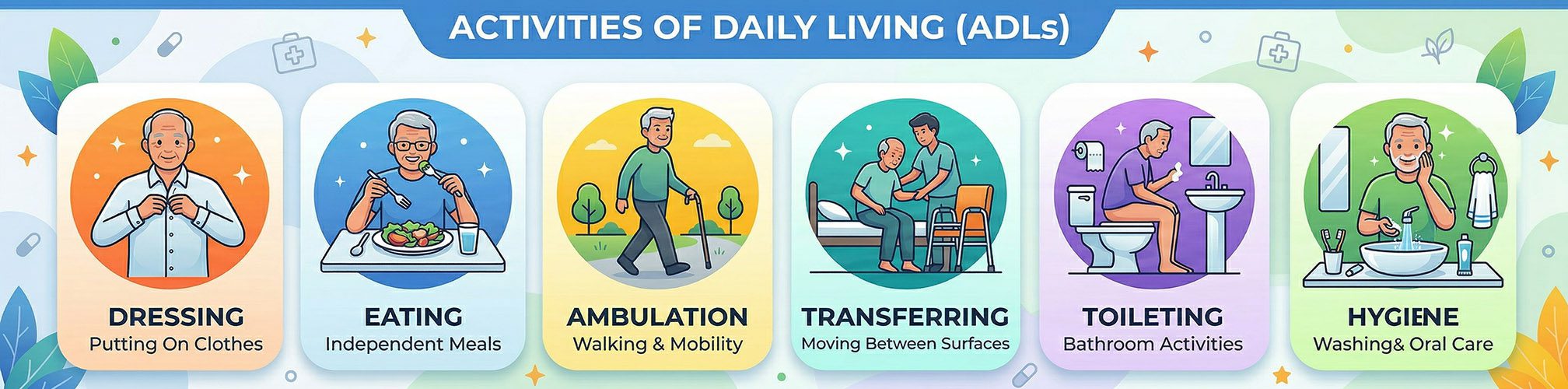
The ADLs are the basic self-care tasks that we initially learn as very young children. They are sometimes referred to as “Basic Activities of Daily Living” (BADLs). They are fundamental for self-care. The activities include:

These are the self-care tasks we usually learn as teenagers. They require more complex thinking skills, including organizational skills. They include:
ADL assessments serve as crucial clinical indicators across various healthcare environments:
Regular ADL monitoring allows healthcare teams to detect subtle functional declines early, potentially preventing more serious health events or unnecessary institutionalization.
You can use the mnemonic words[4] to help you remember.
There are a number of tools to help care professionals assess the ADLs. The common tools as follows:
Feel free to ask for more practical solutions should you need assistance with your loved-one. Our rehabilitation programs will support the Activities of Daily Living.
Physical indicators include unexplained bruising or injuries suggesting falls or mobility problems, declining personal hygiene, and weight loss indicating meal preparation difficulties.
Watch for unsteady gait, balance issues, unusual fatigue during basic tasks, and increased reliance on furniture when walking—all signs that ADL performance is becoming challenging.
Personal hygiene changes often provide early clues of struggles. Look for unwashed hair, body odor, or poor oral hygiene. Clothing choices can reveal problems—repeatedly worn garments, clothes worn inside-out, or weather-inappropriate items.
A reluctance to bathe often develops, with excuses to avoid these activities. These changes typically emerge gradually from physical limitations or cognitive changes affecting task sequencing.
Watch for increased frustration during routine tasks, attempts to hide difficulties, or tasks taking significantly longer to complete. Many people experience withdrawal from social activities due to embarrassment about appearance or concerns about managing toileting away from home.
Some become defensive when offered help, as accepting assistance can feel like surrendering independence.
Consider the frequency of problems—occasional difficulties differ from consistent struggles. Track whether issues are stable or worsening over time. Assess the impact on quality of life—when ADL challenges affect mood, social engagement, or health, they’ve become significant.
Multiple affected ADLs simultaneously typically indicate a more serious situation requiring comprehensive support.
Early mobility indicators include difficulty rising from chairs, reluctance to use stairs, and avoiding rooms requiring step navigation. ‘Furniture walking’—using furniture for stability when moving—is a critical warning sign.
Shortened walking distances, posture changes, or a shuffling gait suggest mobility is becoming compromised in ways affecting ADL performance.
Cognitive changes impact ADL performance even when physical abilities remain intact. You might notice forgotten steps in routines, confusion about everyday objects, or sequencing difficulties when multi-step activities become overwhelming.
Safety concerns arise when cognitive changes affect judgment about hot water, sharp objects, or medication management.
The living environment often reveals difficulties before they’re acknowledged. Look for unopened mail, expired food, unwashed dishes, or neglected housekeeping.
Notice adaptive strategies implemented—clothes laid out in sequences, frequently used items moved to accessible locations, or unused rooms. These modifications often represent attempts to compensate for growing challenges.
Choose a relaxed moment for these sensitive conversations. Use empathetic language focusing on specific concerns rather than generalizations about capability. Frame observations as matters of shared problem-solving rather than criticism.
For example: “I’ve noticed the stairs seem to be giving you trouble. Could we think about ways to make that easier?” Consider involving healthcare professionals who can offer objective assessments.
Healthcare professionals use standardized tools like the Katz Index of Independence or the Barthel Index to objectively evaluate ADL performance. These structured evaluations determine appropriate assistance levels and track changes over time.
Results guide care planning, help families understand current capabilities, and assist in accessing appropriate support services.
With physical limitations, a person typically understands what needs doing but struggles with execution, often devising workarounds. With cognitive decline, they may not recognize necessary tasks or forget midway through activities.
Safety concerns are more prominent with cognitive issues as judgment about risks becomes impaired. Understanding these differences helps provide appropriate support.
Supportive options include home modifications like grab bars and shower benches, assistive devices such as dressing aids and reachers, in-home caregiving, and adult day services.
For comprehensive needs, residential care settings provide structured ADL support while maintaining dignity and quality of life.Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
* References:
[1] https://www.ncbi.nlm.nih.gov/books/NBK470404/
[2] https://hign.org/consultgeri/try-this-series/katz-index-independence-activities-daily-living-adl
[3] https://betterhealthwhileaging.net/what-are-adls-and-iadls/
[4] https://www.timeofcare.com/adl-mnemonic
[5] https://www.alz.org/careplanning/downloads/katz-adl.pdf
[6] https://nursing.ceconnection.com/ovidfiles/00000446-200804000-00023.pdf